Reviewed By: Paul M. Griffey M.D.
November marks Diabetic Eye Disease Awareness Month, a perfect time to learn the intricacies of cataract surgery for diabetic patients. How does diabetes affect cataract surgery and its success?
Drawing from findings by the National Eye Institute, diabetes can significantly influence the outcomes of cataract surgery. This is because certain complications like retinal detachment, vitreous hemorrhage, and infections are more likely to occur in diabetic patients.
It’s also worth noting that many diabetic individuals often battle other health challenges, like heart disease, kidney issues, and lung conditions, that could complicate surgical procedures. Therefore, every patient must ensure their diabetes is well-managed, and their overall health is stable enough for surgery. If you’re a diabetic patient contemplating cataract surgery, a detailed discussion with your doctor about the suitable lens and potential complications is highly recommended.
Table of Contents
What are Cataracts?
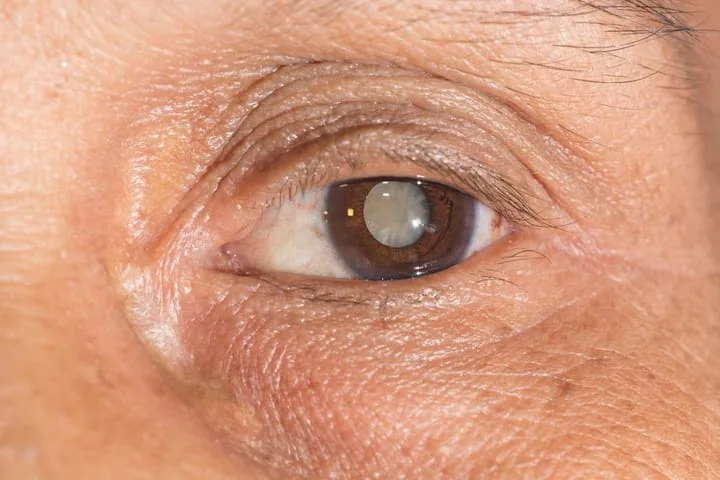
A cataract occurs when the eye’s natural lens becomes clouded. This clouding occurs due to the build-up of proteins that, under normal circumstances, help make up the lens itself. As these proteins degrade, they clump together, creating a cloud-like effect on the lens that blocks your retina’s ability to refract light properly.
Cataracts are more common among older people. As you age, the proteins and fibers in the lens begin to break down and become cloudy. Common symptoms include:
- Blurry vision (also caused by diabetes)
- Faded or yellowing colors
- Poor night vision
- Light sensitivity
- Constant prescription changes
Impact of Diabetes on Cataracts and Cataract Surgery
The interplay between diabetes and cataracts is a subject of concern for medical professionals. The relationship between type 2 diabetes and cataract surgery is significant because diabetes accelerates the formation of protein clumps responsible for cataract development, making cataracts more common in diabetic patients. High blood sugar levels can induce changes in the eye’s lens, leading to the quicker formation of cataracts. This correlation explains why cataracts are a common sight among diabetic patients.
However, other factors like age, smoking, alcohol use, and prolonged exposure to sunlight can also contribute to cataract development, according to the National Center For Biotechnology Information. Diabetic patients noticing symptoms should consult an ophthalmologist to discuss the possibility of cataracts.
So, can a diabetic patient go for cataract surgery? The answer depends on the individual’s overall health and their diabetes management. For diabetes, the experts at Griffey Eye Care recommend laser cataract surgery because of the procedure’s heightened precision and safety.

Diabetic and Concerned About Cataract Surgery? Get the Right Plan
Diabetes affects eye health and healing. Schedule a pre-surgery evaluation to understand how your condition impacts cataract surgery and recovery.
- Comprehensive diabetic eye health review
- Assessing surgical readiness with diabetes
- Tailored post-surgery follow-up schedule
What is the Best Sugar Level for Cataract Surgery?
Maintaining this level is important because high blood sugar levels can lead to multiple complications, negatively impacting the success of the surgery. This is because high blood sugar levels can cause changes to the blood vessels in the eyes, causing conditions like diabetic retinopathy and macular edema to form. Also, elevated blood sugar levels can affect wound healing and increase the risk of infections after surgery.
Regular monitoring and medication adjustments may be necessary to ensure blood sugar levels are within the permissible range for surgery. This active involvement in managing your diabetes will not only contribute to the success of the cataract surgery but also enhance your overall eye health and quality of life.
Light Adjustable Lens (LAL): A Game-Changer for Diabetic Cataract Patients
Here’s where it gets exciting.
For diabetic patients looking for personalized vision correction, Light Adjustable Lenses (LAL) are a groundbreaking innovation worth knowing about.
What is The Light Adjustable Lens?
The Light Adjustable Lens is the first and only intraocular lens (IOL) that can be adjusted after cataract surgery. This technology allows your ophthalmologist to fine-tune your vision post-surgery using ultraviolet (UV) light treatments.
Why is This Especially Important for Diabetic Patients?
Diabetes can make it harder to predict how your eyes will heal and how they’ll respond to standard IOLs. With LAL, there’s flexibility after the surgery to adapt to those healing changes — something that traditional monofocal or multifocal lenses can’t do.
Key Benefits of LAL for Diabetic Patients:
- Post-op customization: Fine-tune your vision weeks after the surgery when your eye has healed.
- Higher satisfaction: Better accuracy in vision outcomes, especially important for diabetics who may have fluctuating eye conditions.
- Reduced need for glasses: Most patients can achieve optimal distance or near vision with minimal dependence on corrective lenses.
Note: Not all patients are candidates for LAL. You must be able to follow post-op UV light treatment protocols. Our eye doctors at Griffey will be able to help determine your eligibility.
How Diabetic Patients Can Choose the Right Lens for Cataract Surgery?
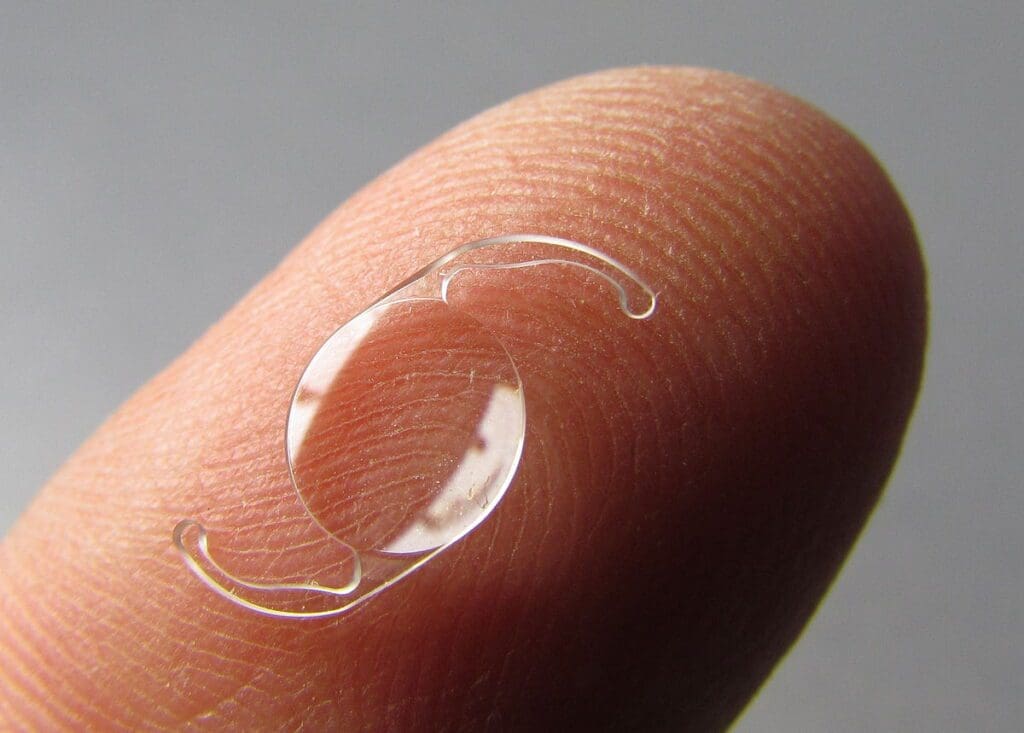
Which lens is suitable for diabetic patients in cataract surgery? Well, every patient has unique vision needs and health situations—so what works for one might not work for another. There are several types of lenses available, including monofocal, multifocal, accommodating, and now Light Adjustable Lenses (LAL) — each having its own advantages and disadvantages.
- Monofocal lenses offer clear vision at a single distance.
- Multifocal lenses provide clarity at multiple distances, often eliminating the need for glasses.
- Accommodating lenses adjust to different distances, mimicking the natural eye’s movement.
- LAL lenses, however, are fully customizable after surgery, offering unique value for patients with complex healing patterns.
Each lens type responds differently to light and can have varying effects on diabetic patients. When choosing the right lens, discuss your lifestyle, vision goals, and specific diabetes-related complications with your ophthalmologist. For example, a multifocal lens might not be suitable if you have diabetic retinopathy due to the potential light distortion.
A Word From Griffey Eye Care
Diabetes can indeed complicate cataract surgeries, but with proper planning, monitoring, and management, successful outcomes can be achieved. If you’re a diabetic patient considering cataract surgery, we urge you to engage in a thorough discussion with your healthcare provider about the different lens options, their implications, and the accompanying risks.
With the advent of Light Adjustable Lenses, there are now more advanced and personalized options than ever before to help you regain clear vision, safely and confidently.
Remember, whatever concerns or questions you may have, Paul M. Griffey, M.D., a specialist in cataracts and glaucoma, is always here to assist you. Let us help you navigate the path toward a clearer vision. Your eye health is our priority. Book your consultation with us today!
**Please note that the suggestions in this blog are for general informational purposes only and may not be suitable for your specific insurance plan and cataract or diabetes needs. It is essential to consult a qualified healthcare professional for personalized advice and treatment.
FAQs: Cataract Surgery and Diabetes
Can I have cataract surgery if I have Type 2 diabetes?
Yes, you can have cataract surgery if you have Type 2 diabetes. However, your blood sugar levels and overall health need to be well-managed before the procedure to reduce potential complications. Discussing your condition with your ophthalmologist is crucial to ensure a safe and effective outcome.
How does my diabetes affect cataract surgery?
Diabetes can increase the risk of complications during and after cataract surgery, such as infections, delayed wound healing, or retinal issues like diabetic retinopathy. Managing your blood sugar levels and addressing any existing eye conditions can help improve surgical outcomes.
Is cataract surgery safe for me if I have diabetes?
Yes, cataract surgery is generally safe for people with diabetes, especially when their condition is well-controlled. Laser-assisted cataract surgery is often recommended for its precision and reduced risk of complications.
Can I have cataract surgery with high blood sugar?
High blood sugar levels can lead to complications, such as poor wound healing or increased infection risk. For a successful surgery, your fasting blood sugar should be less than 140 mg/dL, and postprandial levels should be under 200 mg/dL. Work with your doctor to stabilize your blood sugar before the procedure.
Does my diabetes affect the type of lens I can get for cataract surgery?
Yes, your diabetes can influence lens selection. Certain lenses, like multifocal lenses, might not be suitable if you have diabetic retinopathy or other diabetes-related eye conditions. Discuss your vision goals and health with your doctor to determine the best lens option for you.
What precautions should I take before cataract surgery as a diabetic?
You should:
- Ensure your blood sugar levels are within the recommended range.
- Address any existing diabetic eye conditions, like retinopathy or macular edema.
- Follow your doctor’s advice regarding medications and preparation for surgery.
- Monitor your blood sugar levels closely before and after the procedure.
Why does my diabetes make me more likely to develop cataracts?
Diabetes accelerates cataract formation because high blood sugar can alter the proteins in the lens of your eye, leading to clouding and vision impairment. This makes cataracts more common in people with diabetes compared to those without.